Dr. Vincent Villa – Chirurgien orthopédiste
L’excellence médicale, au service des patients pour le traitement de l’arthrose et des pathologies de l’appareil locomoteur. Nous acceptons les nouveaux patients.
Neuchâtel – Montreux – Genève – La Chaux-de-Fonds
Notre centre est spécialisé dans le
traitement de l’arthrose et des
pathologies de l’appareil locomoteur
Patients traités
dans nos
centres
Années
d’existence
Depuis plus de 10 ans, notre centre ostéo articulaire est un centre de référence dans le traitement de l’arthrose et pathologies de l’appareil locomoteur
Bien préparer, bien vivre et se remettre de son opération
Notre centre ostéo articulaire favorise une expérience positive vous mettant au centre de votre prise en charge. Votre confort est notre priorité et nous vous accompagnons de la prise en charge de vos symptômes jusqu’à votre vie d’après chirurgie. Vous êtes au centre de toutes nos préoccupations.
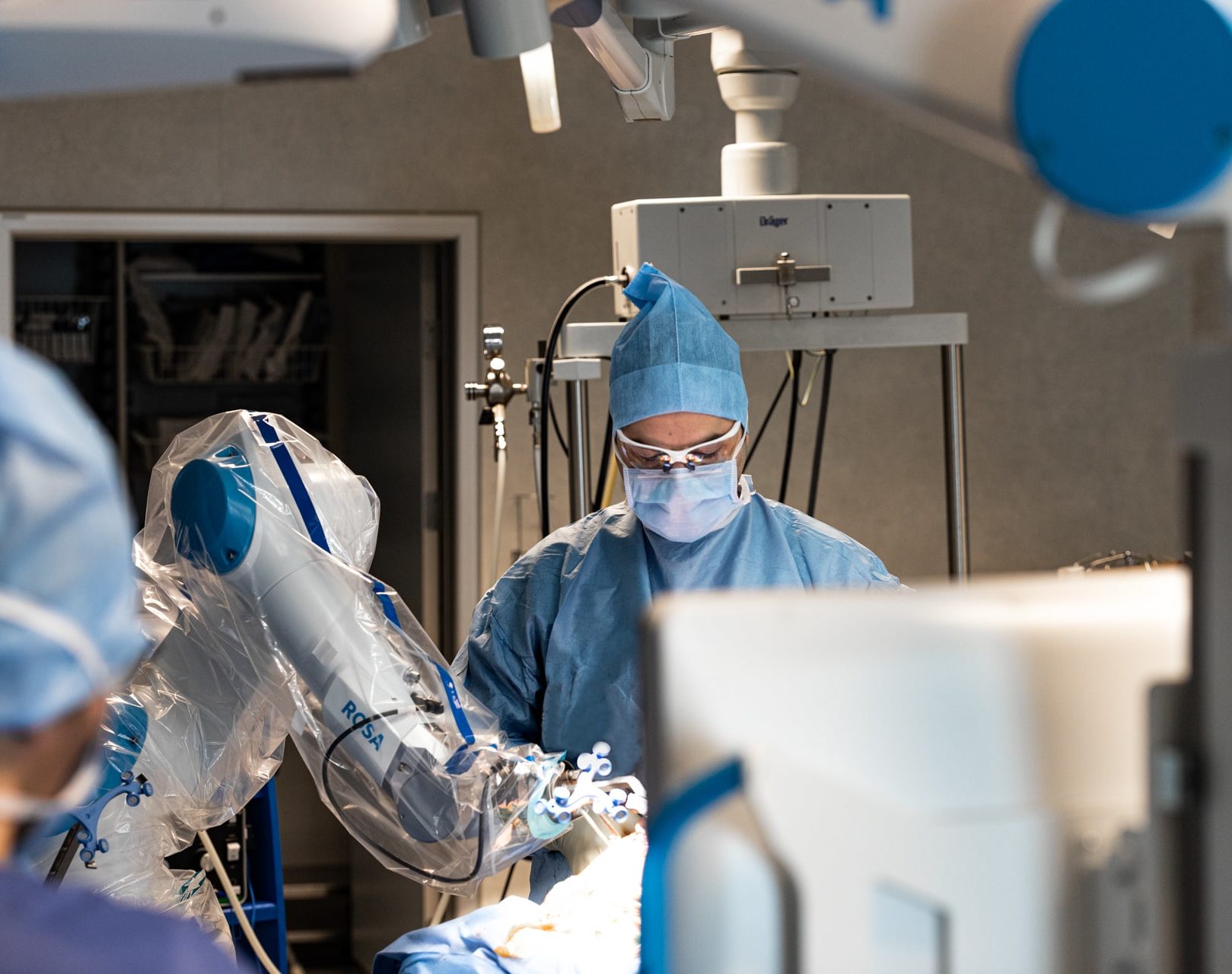

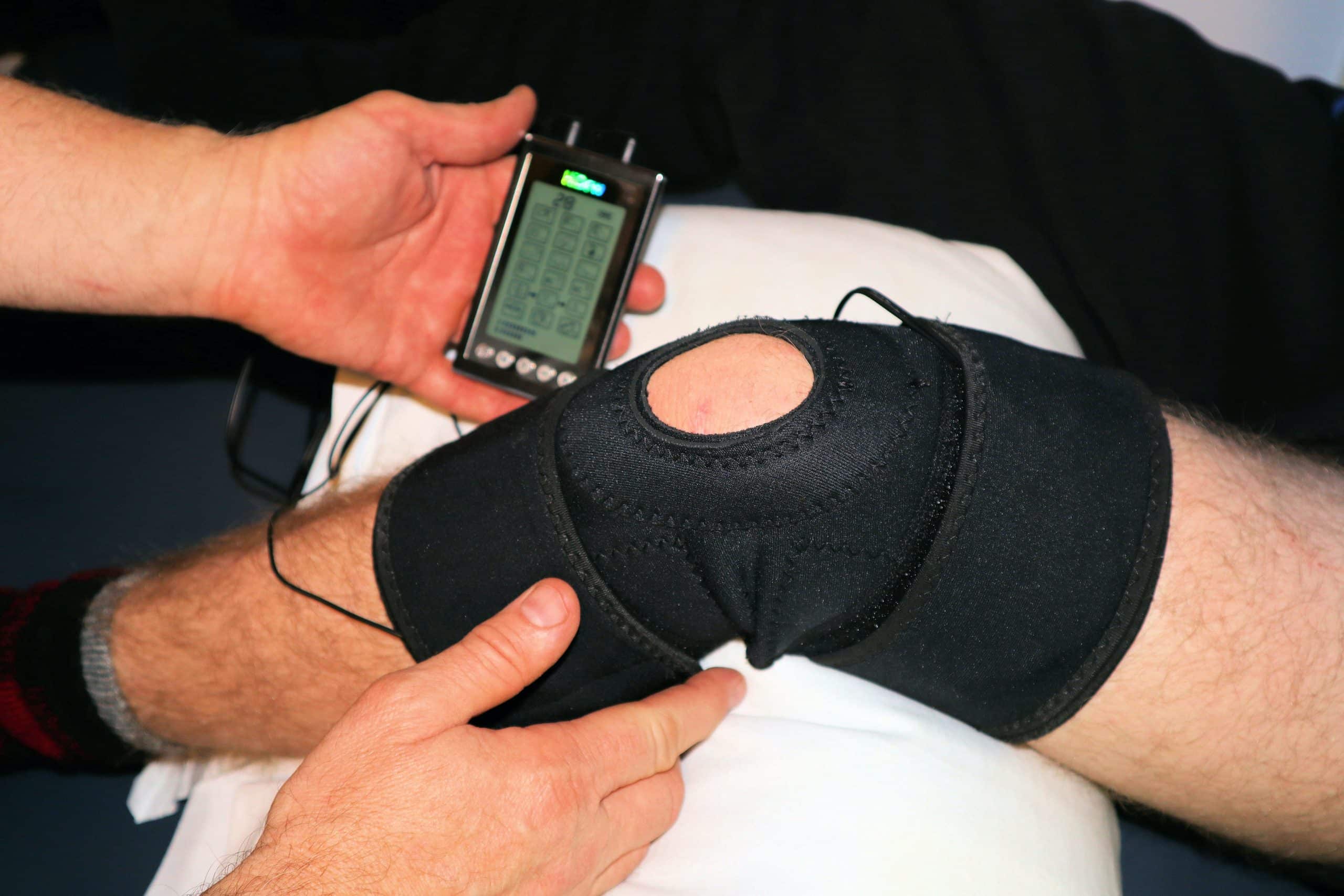

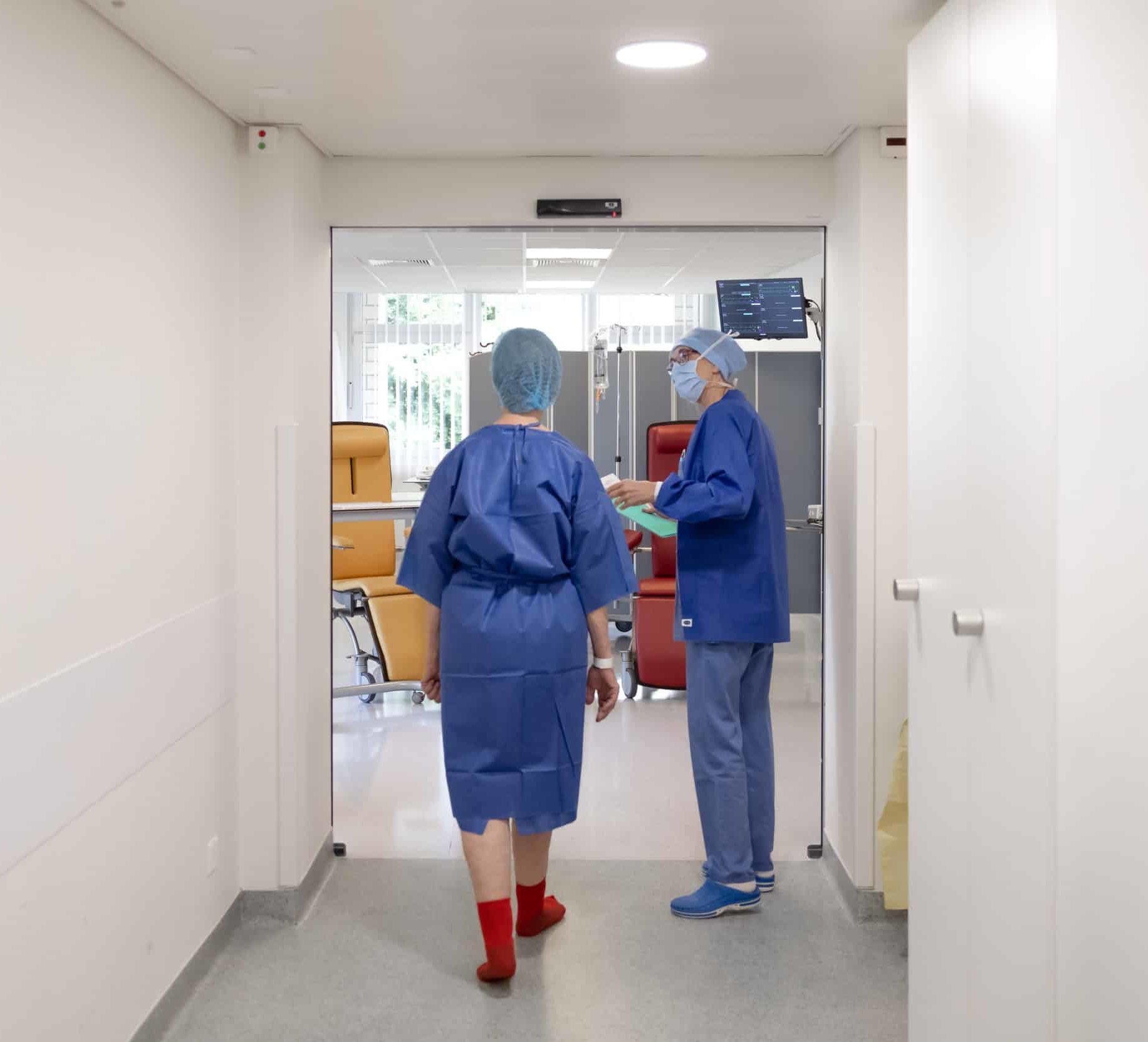
Nos expertises servent le patient avec passion et respect de ses attentes
Les clés de succès d’une bonne prise en charge sont le diagnostic et la prise en charge chirurgicale la mieux adaptée pour le patient, une écoute du patient et de ses sensations, une relation de confiance entre le personnel médical et le patient, une collaboration étroite entre les équipes soignantes, physiothérapeutes, médecins préparateurs physiques, spécialistes en nutrition, club de sport et médecins généralistes dans le respect de la situation du patient.
Traitement de l’arthrose – Chirurgie des ligaments – Chirurgie du membre inférieur – Chirurgie prothétique – Chirurgie du sport – Traitements médicaux – Acide hyaluronique – Drainage Lymphatique – Rotule – Plasma riche en plaquettes
Pathologies
du genou
Pathologies
de la hanche
Le Patient d’abord
Je veux redonner à la chirurgie une dimension plus humaine et toujours apporter le maximum de valeurs et de services aux patients afin d’être partenaire de votre santé
Dr. méd Vincent Villa (FMH)
Chez Liv Ortho, nous souhaitons toujours apporter le maximum de valeurs aux patients ! Notre obsession : augmenter la qualité et la sécurité pour nos patients afin d’être partenaire de votre santé. Nous avons donc imaginé une approche vous mettant au centre de votre prise en charge, respectant vos envies, choix et votre santé. Nous sommes orientés vers le service des patients dans un esprit de confiance et de respect de la vie privée. Nos équipes sont à votre écoute, à chaque instant : le patient d’abord

